Consumer Reports Finds Potentially Harmful Bacteria All Over Chicken Breasts
CR looked at 316 chicken breasts purchased at various types of food retailers, everything from the regionally owned grocery store to national supermarket and big box chains, in 26 different states. The samples covered both name brand products, including Perdue, Pilgrim’s, Sanderson Farms, and Tyson, and conventional no-brand chicken that many of us buy from the poultry section of the market.
Since most chickens produced for the retail market are provided with a steady diet of antibiotics, CR also made sure to test breasts that were labeled as “antibiotic-free” and “organic.” Here is a PDF of every brand included in the tests.
Each breast was tested for the presence of six bacteria — salmonella, campylobacter, staphylococcus aureus, E. coli, enterococcus, and klebsiella pneumoniae. Salmonella, campylobacter and staph are common causes of food poisoning. E. coli and enterococcus are usually the result of fecal contamination, while klebsiella is naturally present in the human stomach but can cause infections like pneumonia.
In addition to determining the mere presence of each bacteria type, CR testers then tried to determine which strains of each pathogen had been found, as one strain of a bug like salmonella may be rather mild while some, like the Heidelberg strain that was behind the recent outbreak, can wreak havoc.
Here are some of the findings:
* There was no significant difference between the average types of bacteria found on conventionally raised chickens (i.e., with antibiotics) and those labeled as “organic” or “no antibiotics.”
* Nearly 80% of the tested samples tested positive for enterococcus, followed by E. coli (65%), campylobacter (43%), klebsiella pneumoniae (13.6%), salmonella (10.8%), then staph (9.2%).
* Of the samples testing positive for E. coli, 17.5% were tainted with the “ExPEC” strain, which is more likely than other types to make a human sick with a urinary-tract infection.
* About half the samples (49.7%) tested positive for at least one multidrug-resistant bacterium, and 11.5% carried two or more types of multidrug-resistant bacteria.
* The drug-resistant bacteria found on the chickens breasts was significantly more resistant to those classes of antibiotics that are FDA-approved for the production (i.e., non-medical) of chickens than for those drugs that are only approved to prevent and treat disease. The FDA recently asked the drug makers to voluntarily stop selling those antibiotics that are solely for production, though farmers would still be feeding their animals all the “preventative” drugs they are now.
Here are some of the results for several name brands, along with the averages for smaller brands and antibiotic-free breasts:
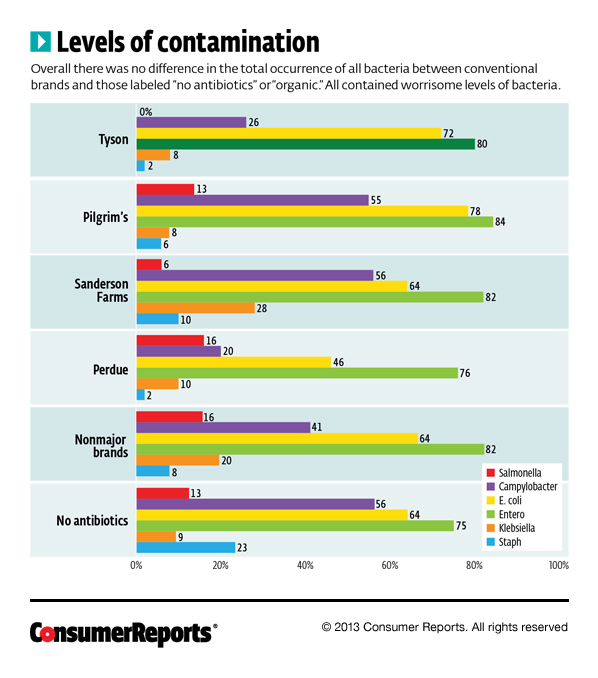
Though most, if not all, of these bacterial issues can be overcome by cooking the chicken breast to an internal temperature of 165° F, that doesn’t get rid of the most common way for humans to contract these food-borne illnesses at home — cross-contamination during the preparation process. You pick up the chicken breast, touch a dinner plate or some utensils without properly cleaning your hands and you may have bought yourself a vacation to Diarrhea Town.
James R. Johnson, M.D., a professor of medicine in the division of infectious diseases at the University of Minnesota tells Consumer Reports that you may be able to pick up one of these bugs just by touching the outside of the packaging.
According to a survey of CR readers, while 82% of Americans say they cook chicken breasts all the way to 165 degrees, only 30% of us actually use a meat thermometer when cooking chicken. More than 9-in-10 Americans claim to wash their hands right after handling raw poultry, but 72% of folks make the mistake of washing chicken before they cook it, when all that’s likely to do is spread bacteria-filled water around your kitchen and onto you.
Here are some more survey findings from the CR story:

Even though both conventionally raised and antibiotic-free chicken breasts contained roughly the same amount of bacteria, choosing antibiotic free is still a smarter choice for public health.
Consumer Reports’ recent tests of packaged ground turkey products found that conventionally raised turkey was more likely to contain drug-resistant bacteria. And choosing meat that is antibiotic free means you are encouraging farmers to not feed their animals drugs that are helping to foster new antibiotic-resistant superbugs that sicken around 2 million Americans and cause more than 23,000 deaths in the U.S. each year.
Among other regulatory and legislative measures, Consumer Reports is calling on Congress to give the USDA authority to recall meat and poultry products that are tied by DNA fingerprinting to disease outbreaks. Amazingly, the agency does not currently have this authority.
Want more consumer news? Visit our parent organization, Consumer Reports, for the latest on scams, recalls, and other consumer issues.


