The White House is working with Republican lawmakers in Congress to revive legislation that would repeal and replace core parts of the Affordable Care Act, but some of the changes being discussed to make this bill more palatable to opponents may take away one of the more popular aspects of the ACA. [More]
pre-existing conditions
Coverage For Pre-Existing Conditions Could Be At Risk In Latest Obamacare Repeal Plan
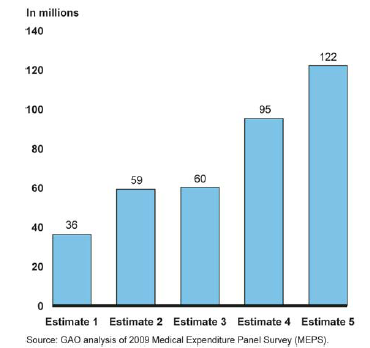
Between 36-122 Million Americans Have Pre-Existing Conditions That Would Restrict Health Insurance Coverage
Health insurance providers have a long history of telling individual policyholders — and people shopping for individual policies — that their care isn’t covered or their policy is voided because of a pre-existing condition. Starting in 2014, that is all supposed to stop when a condition of the Affordable Care Act kicks in, making it illegal for health insurers in the individual market to deny coverage, increase premiums, or restrict benefits because of a pre-existing condition. Question is: Just how many people are we talking about? [More]

Get Insurance Even If You're Uninsured And Have Pre-Existing Conditions
Yesterday healthcare.gov launched which, among many other resources, contains links to where you can apply for the new state high-risk pools which are for uninsured folk with pre-existing conditions. [More]

Skinny Toddlers Also Can't Get Insurance?
We guess we should have seen this one coming. After news broke of the uninsurable fat baby last week, MSNBC found a similar case on the other end of the spectrum. A Colorado family with a 22-pound two-year-old says that United HealthCare told them their daughter Aislin is too small to qualify for insurance under their guidelines.

Fat Little Babies Can't Get Insurance?
Up until yesterday, 4-month-old Alex Lange was considered uninsurable by Rocky Mountain Health Plans because he was above the 95th percentile for height and weight for his age—that gave him a pre-existing condition of obesity, and earned him a stamp of rejection.

