The federal judge overseeing a lawsuit filed by more than a dozen states to stop President Trump’s plan to cut off billions of dollars in payments to health insurance providers has decided to not issue a preliminary injunction preventing the White House from halting the subsidies. [More]
health insurance

Judge Won’t Block Trump’s Plan To Halt Billions In Cost-Sharing Payments To Health Insurers

Trump Cuts Off Billions Of Dollars In Cost-Sharing Payments To Insurers, Putting Obamacare Marketplaces At Risk
Only hours after signing an executive order that undermines several key aspects of the current health care law, President Trump has made good on his repeated threat to pull the plug on billions of dollars in subsidies provided by the federal government to insurers in the individual plan market. [More]
What The Heck Is Single-Payer Healthcare, Anyway?
Health coverage has been in the news in a big way this year, thanks to Republican-led efforts in Congress to repeal the Affordable Care Act (ACA) throughout the spring and summer. That plan ultimately failed, but both sides of the political aisle do agree on one thing: There’s a lot of room to go on improving health care access and containing medical costs. A new rallying cry has risen up among Democrats: Time for single-payer! But what does that actually mean — and what could it look like? [More]

What You Need To Know About Senate Bill To Repeal, Replace Obamacare
After weeks of secrecy, Senate Republican leaders have finally released a draft version of the budget resolution they intend to use to repeal and replace much of the Affordable Care Act. [More]

3 Things We Know About The Senate’s Obamacare Repeal Bill
The Senate — or at least, 13 Republican senators — are currently plugging away at their version of legislation to repeal and replace the Affordable Care Act. Hill-watchers say the goal is to have a vote within the next two weeks, but no drafts of the bill have circulated, no hearings have been held, and all talks are closed-door — so what do we know about the bill? [More]

Walmart To Pay $7.5M After Denying Spousal Benefits To Same-Sex Couples
A federal court judge has approved a $7.5 million settlement between Walmart and current and former employees who claimed that the the retailer unfairly discriminated against them by denying health benefits to their same-sex spouses. [More]
House To Vote On Obamacare Repeal That Could Leave Americans With Pre-Existing Conditions Without Coverage
UPDATE: Both the Washington Post and the Wall Street Journal are now reporting that the House is indeed planning to vote on the repeal measure Thursday. [More]

Appeals Court Upholds Decision To Block $54B Anthem, Cigna Merger
The $54 billion marriage between health insurance behemoths Anthem and Cigna is still off after a federal appeals court denied Anthem’s efforts to overturn a previous court order blocking the mega-merger. [More]

Coverage For Pre-Existing Conditions Could Be At Risk In Latest Obamacare Repeal Plan
The White House is working with Republican lawmakers in Congress to revive legislation that would repeal and replace core parts of the Affordable Care Act, but some of the changes being discussed to make this bill more palatable to opponents may take away one of the more popular aspects of the ACA. [More]

What Are Health Savings Accounts & Why Are They A Big Part Of Obamacare Replacement Plan?
Long before Republican lawmakers unveiled their legislative efforts to repeal and replace the Affordable Care Act, supporters of this movement had talked up “health savings accounts” (HSAs) and how crucial they would be to any eventual Obamacare replacement. What these lawmakers and policy makers often skip over is what an HSA actually is, and whether expanding the use of HSAs will really help most Americans. [More]
Congressional Budget Office: Obamacare Repeal Plan Would Leave 24 Million Additional People Without Insurance By 2026
Two Congressional committees have already passed their legislative efforts to repeal the Affordable Care Act without waiting for feedback from the nonpartisan Congressional Budget Office on how these bills would affect the number of insured in the U.S. The CBO has now released its analysis, concluding that the repeal would result in 14 million fewer people having health insurance in only the first year. After a decade, the CBO estimates that 24 million more people would be without coverage than if the existing plans were kept in place. [More]

Highlights From The House Debate On Tanning Tax That Turned Into A Sideshow
Among the lesser-discussed points of the Affordable Care Act repeal and replace legislation is a move to get rid of a 10% tax on the use of tanning salons. Why is this suddenly an issue, and how did it cause the House Ways and Means Committee’s discussion of the bill to devolve into a sideshow, complete with debates on the merits of ice cream and Spain’s tax on the sun? [More]

Report: Obamacare Replacement Will Likely Cover Fewer Americans
So far, the only thing the White House has said about its plans to replace the Affordable Care Act is that it would provide “insurance for everyone” and that people would be “beautifully covered,” but comments coming out of Washington indicate that not everyone will be able to obtain coverage under the replacement plan. [More]

Federal Judge Blocks $54 Billion Anthem/Cigna Merger
Only a few weeks after a federal court blocked the insurance mega-merger of Aetna and Humana, it’s happened again: Last night, a U.S. District Court judge rejected the $54 billion marriage of health insurance giants Anthem and Cigna. [More]
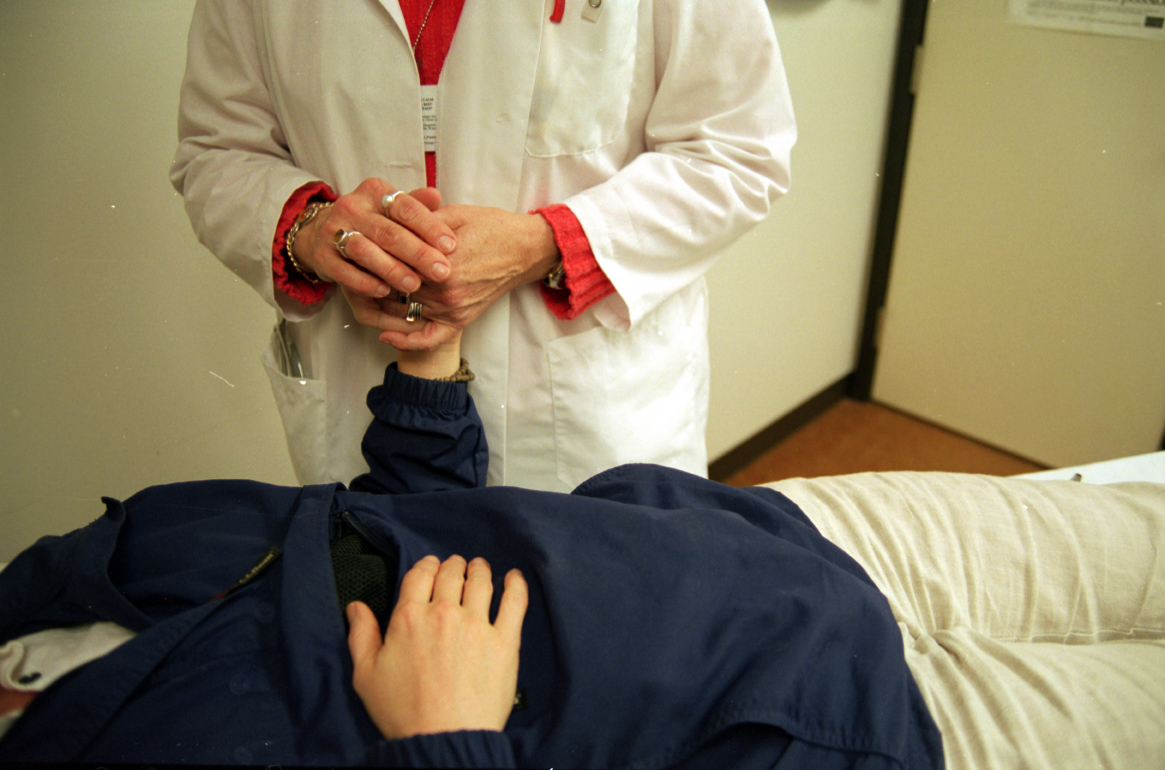
Hospitals To Congress: Keep Obamacare Or Restore Billions In Payments To Cover Uninsured
When a patient shows up to the emergency room needing immediate life-saving surgery, they are going to receive treatment whether they have insurance or not. With both Congress and the White House pushing for repeal of the Affordable Care Act, hospital administrators are telling lawmakers they will need to restore billions of dollars a year in federal funding to hospitals to cover the costs of treating uninsured and low-income patients. [More]
Aetna And Humana May Appeal Ruling Blocking Their Merger
This week, a federal judge blocked the proposed $37 billion merger of health insurance giants Aetna and Humana, ruling that the two companies would significantly reduce competition in the health care market if they teamed up. Now what are the two companies going to do? They might appeal the ruling. Or not. [More]
Federal Judge Blocks $37 Billion Merger Of Aetna & Humana
Six months after the U.S. Department of Justice and attorneys general from eight states and the District of Columbia sued to stop the merger of insurance giants Aetna and Humana, the federal judge in the case has blocked the deal from moving forward. [More]


